Scientists Convert Type A Blood to Universal Donor Blood
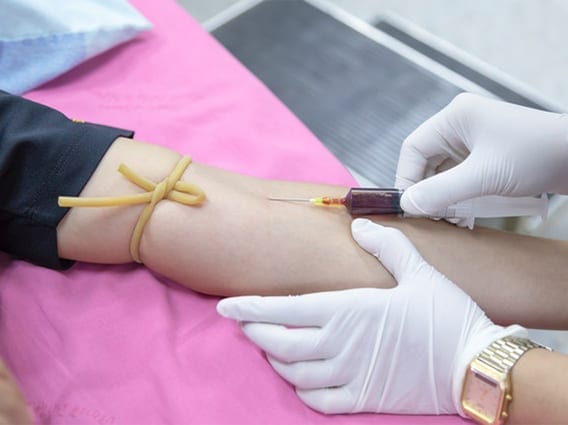
Between scheduled operations, routine transfusions, and emergency operations someone in the United States needs blood every two seconds. Unfortunately, however, recipients can’t just accept any blood; patient and donor blood types must be compatible. Until now, Type O blood was the only red cell universal donor, but researchers analyzing bacteria in the human gut have discovered that microbes there produce two enzymes that can convert Type A blood into a universally accepted type, Science magazine reports.
“This is a first, and if these data can be replicated, it is certainly a major advance,” Harvey Klein, a blood transfusion expert at the National Institutesof Health’s Clinical Center in Bethesda, Maryland.
Previous research had been conducted on Type A blood, but had been met with little success. After 4 years, a team from the University of British Columbia decided, rather than continue to try and adapt the known enzyme capable of removing “A-defining” antigens, to look to human gut bacteria for a better solution. While initially the team did not see much success, when they tested two enzymes at once, the sugar molecules that define a blood type were effectively removed.
“They findings are very promising in terms of their practical utility,” Mohandra Narla, a red blood cell physiologist at the New York Blood Center, said. While more testing will need to be done to ensure that all Type A antigens have been completely removed, if this research proves truly successful, the availability of “universal” donor blood could nearly double.